Note: This article will update as we learn more, and to reflect any changes that may happen before the rule is officially published to the Federal Register on November 23, 2018. To view the entirety of the final rule, view the unpublished pdf version.

Last night CMS released the Final Rule for the third year of the Quality Payment Program. As has been the case in the prior two years of reporting, two tracks are offered for successful participation: the Merit-Based Incentive Payment System (MIPS) and Advanced Alternative Payment Models (Advanced APMs). This summary will focus on the MIPS track of the QPP.
RELATED: 2019 MIPS Reporting Quick-Reference Sheet
1. The Basics of MIPS Reporting in 2019
Eligible Clinicians
Eligible clinician types are expanding for 2019 reporting, now to include:
- Physical Therapists
- Occupational Therapists
- Clinical Psychologists
- Qualified Speech-Language Pathologists
- Qualified Audiologists
- Registered Dieticians and Nutrition Professionals
Notably missing from this list are Clinical Social Workers, who were considered eligible in the proposed rule, but who became exempted based on feedback CMS obtained during the comment period. Newly eligible clinician types are exempt from the Promoting Interoperability performance category.
Additionally, the low-volume threshold will be changing slightly. Now clinicians that have ≤ $90,000 in Medicare Part B charges -OR- ≤ 200 Medicare Part B beneficiaries -OR- ≤ 200 covered professional services under the Physician Fee Schedule (PFS) do NOT have to participate in MIPS. A new option this year is for clinicians who fall under this threshold to participate if they opt to.
MIPS Final Score Weighting
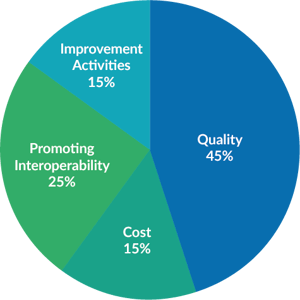 Cost continues to be worth more when compared to the prior reporting year, now weighted as 15% of participant's MIPS final score. Quality has also been adjusted to be worth 45% for 2019 reporting. Promoting Interoperability (25%) and Improvement Activities (15%) will remain the same weight as they were in 2018.
Cost continues to be worth more when compared to the prior reporting year, now weighted as 15% of participant's MIPS final score. Quality has also been adjusted to be worth 45% for 2019 reporting. Promoting Interoperability (25%) and Improvement Activities (15%) will remain the same weight as they were in 2018.
The performance thresholds for 2019 have become slightly more challenging:
- 0-29%: Below minimum performance threshold. Will result in a -7% penalty.
- 30-74%: Acceptable performance. Penalty will be avoided, and up to a 7% incentive is possible.
- 75%+: Exceptional performance. Penalty will be avoided, participants will be eligible for the 7% incentive + a possible extra 10% for exceptional performance.
2. Quality Performance Category
Category Requirements
The basic requirements of the Quality performance category aren't changing much when compared with 2018 reporting. Participants still must report six quality measures, one of which is an outcome measure. If not outcome measures apply, a high-priority measure may be used in its place. Alternatively, participants can report six measures from a specialty-specific measure set or a subspecialty specific-measure set. If less than six measures are included in the selected measure set, then all measures in the set must be reported.
For all QCDR measures, MIPS CQMs, and eCQMs, the data completeness threshold for quality measures is remaining at 60 percent. In other words, for performance data for a measure to be considered complete, at least 60% of the eligible patients or patient visits for the full year (as defined in the specifications of the selected measure) must be reported. Eligible patients continue to include patients seem from all payers.
Facility-Based Measures
Facility-based measures will be available for use in 2019. (more details forthcoming)
Added and Removed Quality Measures
Ten new measures will be introduced:
- #468: Continuity of Pharmacotherapy for Opioid Use Disorder
- #469: Average Change in Functional Status Following Lumbar Spine Fusion Surgery
- #470: Average Change in Functional Status Following Total Knee Replacement Surgery
- #471: Average Change in Functional Status Following Lumbar Discectomy Laminotomy Surgery
- #472: Appropriate Use of DXA Scans in Women Under 65 Years Who Do Not Meet the Risk Factor Profile for Osteoporotic Fracture
- #473: Average Change in Leg Pain Following Lumbar Spine Fusion Surgery
- #474: Zoster (Shingles) Vaccination
- #475: HIV Screening
- (No Quality #): Ischemic Vascular Disease Use of Aspirin or Anti-platelet Medication
- (No Quality #):Falls: Screening, Risk-Assessment, and Plan of Care to Prevent Future Falls
For more details about these new measures, please refer to Table A of Appendix 1: Finalized MIPS Quality Measures. We will be providing further details about them when the full specifications are released in December.
Additionally, 26 measures will be removed:
- #88: Diabetic Retinopathy: Documentation of Presence or Absence of Macular Edema and Level of Severity of Retinopathy
- #134: Coronary Artery Bypass Graft (CABG): Use of Internal Mammary Artery (IMA) in Patients with Isolated CABG Surgery
- #99: Breast Cancer Resection Pathology Reporting: pT Category (Primary Tumor) and pN Category (Regional Lymph Nodes) with Histologic Grade
- #100: Colorectal Cancer Resection Pathology Reporting: pT Category (Primary Tumor) and pN Category (Regional Lymph Nodes) with Histologic Grade
- #122: Adult Kidney Disease: Blood Pressure Management
- #140: Age-Related Macular Degeneration (AMD): Counseling on Antioxidant Supplement
- #156: Oncology: Radiation Dose Limits to Normal Tissues
- #163: Comprehensive Diabetes Care: Foot Exam
- #205: Ischemic Vascular Disease (IVD): Use of Aspirin or Another Antiplatelet
- #224: Melanoma: Avoidance of Overutilization of Imaging Studies
- #251: Quantitative Immunohistochemical (IHC) Evaluation of Human Epidermal Growth Factor Receptor 2 Testing (HER2) for Breast Cancer Patients
- #257: Statin Therapy at Discharge after Lower Extremity Bypass (LEB)
- #263: Preoperative Diagnosis of Breast Cancer
- #276: Sleep Apnea: Assessment of Sleep Symptoms
- #278: Sleep Apnea: Positive Airway Pressure Therapy Prescribed
- #327: Pediatric Kidney Disease: Adequacy of Volume Management
- #334: Adult Sinusitis: More than One Computerized Tomography (CT) Scan Within 90 Days for Chronic Sinusitis (Overuse)
- #359: Optimizing Patient Exposure to Ionizing Radiation: Utilization of a Standardized Nomenclature for Computed Tomography (CT) Imaging
- #363: Optimizing Patient Exposure to Ionizing Radiation: Search for Prior Computed Tomography (CT) Studies Through a Secure, Authorized, Media-Free, Shared Archive
- #367: Bipolar Disorder and Major Depression: Appraisal for alcohol or chemical substance use
- #369: Pregnant women that had HBsAg testing
- #373: Hypertension: Improvement in Blood Pressure
- #423: Perioperative Anti-platelet Therapy for Patients Undergoing Carotid Endarterectomy
- #426: Post-Anesthetic Transfer of Care Measure: Procedure Room to a Post Anesthesia Care Unit (PACU)
- #427: Post-Anesthetic Transfer of Care: Use of Checklist or Protocol for Direct Transfer of Care from Procedure Room to Intensive Care Unit (ICU)
- #447: Chlamydia Screening and Follow-up
Rationale for removal can be found in Table C of Appendix 1: Finalized MIPS Quality Measures. Generally speaking, measures were removed if they were extremely topped out (consistent performance rate between 98-100%), duplicative, not connected to improved outcomes, or not demonstrating variation in performance.
RELATED: Register for an upcoming webinar covering 2019 MIPS
3. Cost Performance Category
Category Requirements
Cost measure performance is captured automatically via administrative claims, so no additional submission is required. The two measures that are being utilized to determine participants 2018 Cost score, total per capita cost and Medicare spending per beneficiary, will continue to be used in 2019. Additionally, eight episode-based measures will be introduced.
Episode-Based Cost Measures
CMS developed and tested eight episode-based cost measures during the 2018 performance year, representative of the cost to Medicare for items and services furnished to a patient during an episode of care. These new measures are calculated using Medicare Parts A and B FFS claims data.
| Measure Topic | Measure Type |
|---|---|
| Elective Outpatient Percutaneous Coronary Intervention (PCI) | Procedural |
| Knee Arthroplasty | Procedural |
| Revascularization for Lower Extremity Chronic Critical Limb Ischemia | Procedural |
| Routine Cataract Removal with Intraocular Lens (IOL) Implantation | Procedural |
| Screening/Surveillance Colonoscopy | Procedural |
| Intracranial Hemorrhage or Cerebral Infarction | Acute inpatient medical condition |
| Simple Pneumonia with Hospitalization | Acute inpatient medical condition |
| ST-Elevation Myocardial Infarction (STEMI) with Percutaneous Coronary Intervention (PCI) | Acute inpatient medical condition |
4. Improvement Activities Performance Category
Category Requirements
The base requirements for the Improvement Activities performance category have changed very little. The category will still be worth 15% of the MIPS final score, with full credit awarded to participants who achieve 40 points (20 points for small or rural practices, HPSAs, non-patient facing clinicians, or APM participants). Medium-weight activities remain worth 10 points, and high-weight activities worth 20 points.
Added, Modified, and Removed Improvement Activities
There are 6 new improvement activities available for attestation in 2019:
- IA_AHE_7: Comprehensive Eye Exams (Medium)
- IA_BE_24: Financial Navigation Program (Medium)
- IA_BMH_10: Completion of Collaborative Care Management Training Program (Medium)
- IA_CC_18: Relationship-Centered Communication (Medium)
- IA_PSPA_31: Patient Medication Risk Education (High)
- IA_PSPA_32: Patient Safety and Practice Assessment (High)
Additionally, 1 activity has been retired:
- IA_PM_9: Participation in Population Health Research
5. Promoting Interoperability Performance Category
Category Requirements
The most obvious change to this category is found in its name - the category previously known as Advancing Care Information is now called Promoting Interoperability. However, the most impactful change that has been finalized for 2019 is the requirement to use 2015 Edition CEHRT.
PI Measures
- E-Prescribing
- Provide Patient Access
- Request / Accept Summary of Care
- Security Risk Analysis
- Send a Summary of Care
- Clinical Data Registry (CDR) Reporting
- Clinical Information Reconciliation
- Electronic Case Reporting
- Immunization Registry Reporting
- Patient-Generated Health Data
- Patient Specific Education
- Public Health Registry Reporting
- Secure Messaging
- Syndromic Surveillance Reporting
- View, Download, or Transmit (VDT)
- Opioid Treatment Agreement
- Query of PDMP
