The NAACOS Fall 2021 Conference was the first live meeting that the Healthmonix team attended since HIMSS 2020 was cancelled in March of that year. It was certainly reinvigorating to meet in person, discuss the state of payment models, and hear from CMS regarding their vision.
Topics: CMS, ACO, Industry insights, 2021 PFS Proposed Rule
There has been much talk around MVPs in the CMS quality reporting arena. MVP means MIPS Value Pathway, and it’s a reporting framework that CMS is communicating as (a) the next evolution of MIPS and (b) a transition tool for getting to other alternative payment modules. As CMS continues to define and refine their vision of the MVPs, they have started to call the current framework 'traditional MIPS' to prepare for the inclusion of the MVP option. You’ll see this when you visit the QPP site. That said, how can MVPs affect MIPS?
Topics: MACRA & MIPS, CMS, 2021 PFS Proposed Rule, MIPS Value Pathways
The 2021 Final Rule: New Programs, Higher Standards and COVID-19
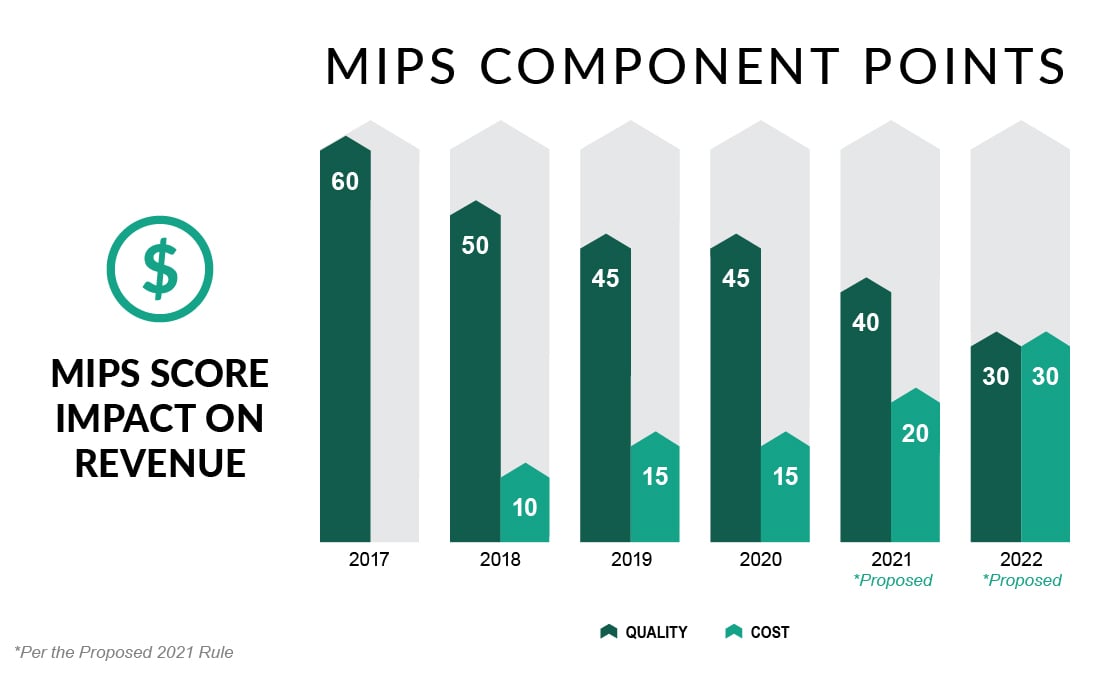
The long-awaited CY 2021 Medicare Physician Fee Schedule Final Rule update is now here. Despite the disruptions of the Public Health Emergency COVID-19, participation in performance year 2019 was strong. Thus the 2021 Final Rule moved forward with finalizing a number of proposed changes, including a higher performance threshold for performance year 2021, anticipated changes in weight to the Quality and Cost performance categories of the Merit-based Incentive Payment System (MIPS), and the introduction of the APM Performance Pathway. Other expected initiatives, such as MIPS Value Pathways, the requirement for registries to build their own benchmarks for certain measures, and the sunsetting of the CMS Web Interface, have been pushed back to at least the 2022 performance year.
Topics: MACRA & MIPS, APMs, COVID-19, 2021 PFS Proposed Rule, APM Performance Pathway
The 2021 Proposed Rule was released last week, and there are some potential changes that you should keep your eye on. Scouring through the entire release, it’s apparent that the Centers for Medicare & Medicaid Services (CMS) kept to their two main objectives:
- Minimize changes to reduce the burden on providers digging out of COVID-19
- Keep the momentum of the Quality Payment program moving forward
Topics: MACRA & MIPS, CMS, Policy, 2021 PFS Proposed Rule