 The 2021 Proposed Rule was released last week, and there are some potential changes that you should keep your eye on. Scouring through the entire release, it’s apparent that the Centers for Medicare & Medicaid Services (CMS) kept to their two main objectives:
The 2021 Proposed Rule was released last week, and there are some potential changes that you should keep your eye on. Scouring through the entire release, it’s apparent that the Centers for Medicare & Medicaid Services (CMS) kept to their two main objectives:
- Minimize changes to reduce the burden on providers digging out of COVID-19
- Keep the momentum of the Quality Payment program moving forward
- Delay MIPS Value Pathways (MVPs): Under this proposal, the MIPS Value Pathways (MVPs) will not be introduced until the 2022 performance period. The MVPs are designed to align each MIPS participant with measures that are more suitable to their specialty and work. The program would encompass all four MIPS categories and utilize measures for each to represent the providers’ work more accurately. CMS will be utilizing this delay in implementation of the MVPs to refine the program and garner more feedback.
- Introduce the APM Performance Pathway (APP): CMS is proposing a new Pathway for their Alternative Payment Models (APMs) providers. This will be a reporting option for those providers that are reporting as part of an APM. The program significantly reduces the variables in quality reporting reducing the number of measures to six standardized measures. The idea is to show the impact of the APM groups more accurately by concentrating on the population health of the community they serve. In some ways, this is similar to the MVP program that will be launched in future years for MIPS. CMS is working towards a simplified, more uniform reporting structure.
- Eliminate Web Interface reporting: CMS proposes the elimination of the Web Interface reporting mechanism. APM participants will either report through the APP (as described above) or they will report MIPS measures through one of the available mechanisms. Those MIPS providers who in the past reported through the Web Interface will now need to report utilizing a registry like MIPSpro® or their Electronic Health Record (EHR).
- Change Quality category: For the Quality category in the 2021 performance year, CMS is proposing to use current year data to benchmark quality measures. Their belief is that 2019 and 2020 data will be skewed due to COVID-19. This will make it more difficult to predict MIPS quality scores as benchmarking drastically impacts measure scoring. Tracking data and utilizing products from a large registry like MIPSpro® will help providers get a better perspective on what their score will be.
![]()
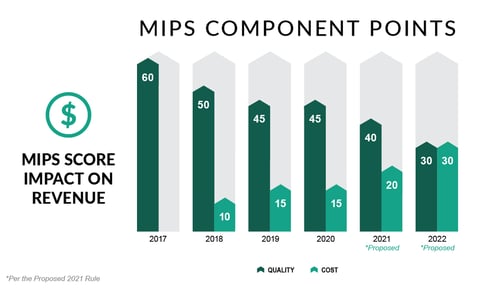
- Increase Cost category weight: The Cost category under MIPS will now be worth 20% of a provider’s overall score under this proposed rule. This change is a step in the direction to make Quality and Cost equal by 2022 as it is mandated by law. The Cost category should be something that every provider starts paying attention to as the MVP program will usher in more specialty specific measures comes 2022, making more provider types eligible for this category.
- Updates for telehealth: Overall, CMS is embracing telehealth through each of the MIPS categories. They see telehealth as not only a 2020 phenomenon, but as a trend that will impact healthcare moving forward. They are also continuing their yearly changes to quality measures. They will be adding, eliminating, and changing several measures that will impact a provider’s options for reporting.
So, what are the key takeaways?
- MIPS is not going anywhere – The program will continue to expand on the current options and will continue to introduce new programs and alternatives moving forward.
- Track and improve your scores – Between measure changes and scoring changes, understanding where you stand throughout the year will be more important moving forward. The impact will grow as well. The proposed rule is looking at a 50% threshold to avoid the penalty of up to 9%, which will result in a smaller group that will achieve the maximum reimbursement. Speaking of reimbursement, CMS is predicting the top performers will receive upwards of 6.89% (the highest mark since MIPS started).
- Growth in importance of the Cost Category – CMS has given a reprieve for specialist by delaying the introduction of the MVP program till 2022. This will reduce the burden on those providers for this upcoming year, however it will give CMS more time to deliver a more impactful program. Otherwise, Cost is moving full steam ahead. With the increase to 20% of a provider’s overall score and the elevation of telehealth measures, the Cost impact will drive your MIPS scores more than ever before.
For more information, we will be having a webinar next week to discuss the proposed changes and how it will impact MIPS moving forward.
To learn more about how MIPSpro can help you navigate those changes, please visit us at www.mipspro.com.
