If you are a dermatology practice, you probably breathed a sigh of relief when the Centers for Medicare & Medicaid Services (CMS) announced that dermatologists, along with many other specialists, would no longer be attributed patients for the Total per Capita Cost (TPCC) measure, as part of the Cost component of the Merit-based Incentive Payment System (MIPS). However, in 2022, CMS introduced a Melanoma Resection Cost measure that is attributed to those specialists that perform these resections. So the Cost category is back for many dermatologists. Even if this is the only Cost measure that is attributed to your practice, it is worth 30 of your total 100 MIPS points - as much as all your Quality measures combined!
The basic qualification for this measure is that a TIN or TIN/NPI bill have at least 10 procedures in the following list with an accompanying diagnosis of either malignant melanoma (C43) or melanoma in situ (D03). MOHS surgery is not included in the procedures that qualify for this measure.
|
CPT/HCPCS |
Description |
|
11600 - 11604, 11606 |
Removal of malignant growth for the trunk, arms, or legs |
|
11620 - 11624, 11626 |
Removal of malignant growth of the scalp, neck, hands, feet, or genitals |
|
11640 - 11644, 11646 |
Removal of malignant growth of the face, ears, eyelids, nose, or lips |
|
14000, 14001, 14020, 14021, 14040, 14041, 14060, 14061, 14301 |
Tissue transfer of the trunk, scalp, arms, legs, forehead, cheeks, chin, mouth, neck, underarms, genitals, hands, feet, eyelids, nose, ears, and/or lips |
When a TIN meets this threshold, CMS will calculate the cost of all episodes attributed, risk adjust those episodes and assign a score to the measure for the Cost category. The measure score is the average risk-adjusted cost across all attributed episodes for the episode group.
What Costs Are Included?
For each procedure that meets the criteria billed above, an episode of care is triggered. CMS will look for all related costs billed by the TIN and all other providers for that procedure. This includes all costs from 30 days prior to the procedure to 90 days after the procedure. CMS has worked with specialists to determine what costs to include. All costs that are billed in relation to the diagnoses of either malignant melanoma (C43) or melanoma in situ (D03) will be billed. This includes surgery, anesthesia, office visits, ED and inpatient stays, and other related services. For example, if a sentinel node biopsy is done within 90 days, that will be included. If the patient has an inpatient stay related to melanoma, that will be included, however if the stay is not related to this diagnosis, those costs will not show in the episode.
According to the literature and feedback received through stakeholder input activities, this measure’s focus represents an area where there are opportunities for improvement. As discussed in the rest of this section, primary opportunities for improving melanoma resection cost outcomes include selectively performing sentinel lymph node (SLN) biopsies, performing follow-up procedures as close as possible together, and reducing downstream complications through adherence to clinical guidelines.
More selectively performing SLN biopsies (i.e., not performing them for all melanomas) will allow for cost savings due to fewer procedural costs for SLN services, as well as fewer complications due to additional procedures. The SLN biopsy is a procedure frequently performed after a melanoma excision, when the size of the melanoma indicates potential disease spread. The SLN biopsy can confirm presence and absence of metastases, where a positive SLN biopsy result indicates non-localized and thus more severe disease (regional/distant). Performing this procedure may assist in long-term disease-free survival, as the SLN procedure can identify nodal metastases that would be otherwise caught later via other methods of observation, such as monitoring. This is corroborated by one study that found that the 10-year disease-free survival rate for those that underwent an SLN biopsy were significantly greater than those that were simply monitored for melanoma recurrence in lymph nodes. However, due to costs and the nearly triple complication rate of SLN biopsies compared to standard melanoma resections, these procedures should only be used selectively. One meta- analysis suggested that early-stage melanomas (Stage 1 or less) should not be followed routinely by an SLN biopsy, as the risks outweigh the benefits of the procedure. At an early stage, the patient is less likely to have metastases to be removed, meaning that the only benefits are confirming no disease presence, while adding risk through exposing the patient to potential surgical complications.
As another example of opportunity for improvement, research suggests that the timing of primary excision and secondary reconstructive procedures may contribute to better cost outcomes. One study indicated that roughly 20% of Medicare patients undergoing surgical treatment to remove a melanoma experience a delay of longer than 1.5 months between biopsy and excision procedure, with longer delays being correlated with higher morbidity and mortality compared to excising within 30 days of biopsy. This is especially true for early-stage melanomas, which are the intended scope of the Melanoma Resection measure. Minimizing delays between the excision of the melanoma and reconstructive procedures may also lead to opportunities for improvement. One study suggested that performing the reconstructive procedure immediately after excision can generate substantial savings, especially in the inpatient setting, noting a 38.5% lower cost in the treatment arc with immediate reconstruction compared to the cost of delayed reconstruction. While immediate reconstruction could potentially allow a reconstructed wound to have residual disease, the paper notes an acceptably low rate of residual tumors requiring operation.
Beyond timing of procedures, focusing on other ways to reduce downstream complications relevant to the index melanoma resection presents an opportunity to lower the cost of care. These complications can include surgical site infections (SSIs), delayed wound healing or wound dehiscence, as well as skin grafts or skin substitutes. While clinical characteristics may predispose certain patients to SSIs, the likelihood of an SSI can be reduced through evidence-based practices. These practices include, but are not limited to, proper administration of any necessary antibiotics and appropriate use of medical and sanitary equipment by the medical staff, including wearing proper surgical attire and disinfecting the surgical site prior to excision. Adhering to these evidence-based practices mitigates common post-operative complications, such as infection and wound dehiscence, which require follow-up and additional treatment outside of the standard treatment arc of a melanoma resection.
Given the incidence and mortality of melanoma in the Medicare-aged population, the Melanoma Resection measure represents an opportunity to control Medicare spending for melanoma as the incidence of melanoma rises. In the United States, the average age when melanoma is diagnosed is 65, with incidence and melanoma-specific mortality increasing with age and peaking in those aged 65-74 years. It is estimated that 196,060 cases of melanoma will be newly diagnosed in 2020. Furthermore, it is estimated that the total annual treatment costs for melanoma are $3.3 billion annually, a figure that is anticipated to continue to rise due to the increasing incidence of melanoma.
Some sample episodes of care:
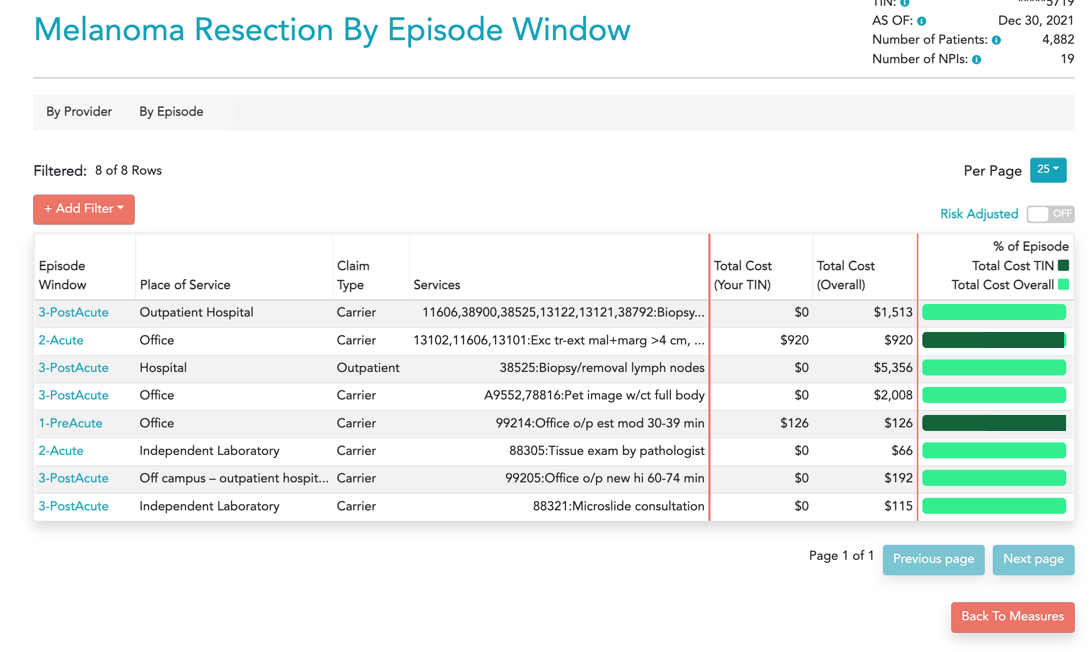
Case 1 – An excision (CPTs 13121, 11603) with a pathology exam (CPTs 88305, 88342) for a total cost of $738. Low cost episode with good outcome:
%20with%20a%20pathology%20exam%2012-8.png?width=1078&height=525&name=An%20excision%20(CPTs%2013121%2c%2011603)%20with%20a%20pathology%20exam%2012-8.png)
Case 2 – An excision followed by a sentinel node biopsy and additional services. Total episode cost is $10,296. This episode is very high cost due to the need for additional imaging and SLN biopsy:
Case 3 – An excision followed by a wound complication, resulting in a total episode cost of $21,958.
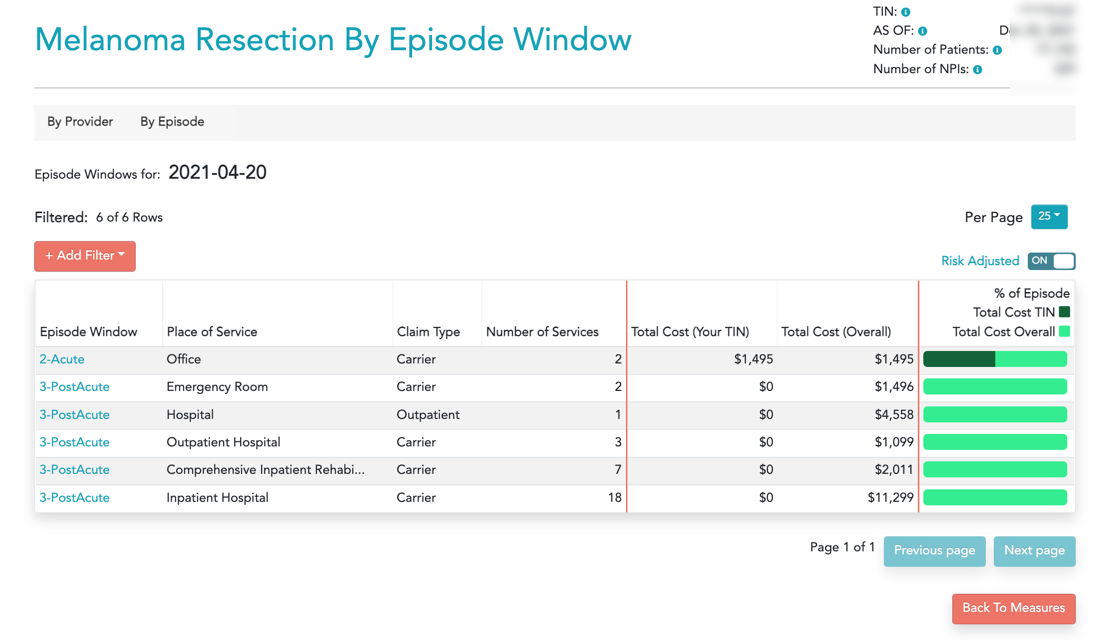
Note that the differences in the episode costs are significant. Healthmonix can assist dermatologists in providing this data and analyzing where areas for improvement exist. Contact us to learn more.

