As you report your MIPS data, it can feel like a lot of work with little ROI for the last two years. But wait. Sometimes we need to step back and evaluate the bigger picture. While we often focus on "getting the job done", there are changes in the healthcare economy that are occurring that are strategic.

Here are some impacts from your MIPS reporting that need consideration as we move forward into 2022.
Reputation with employers. MIPS scores follow a physician as they transition from practice to practice. They continue to impact reimbursement for the new practice in following years. Several of our clients have reported checking MIPS scores as they acquire or work with other practices. Reputation can be an impact when negotiating contracts or hiring.
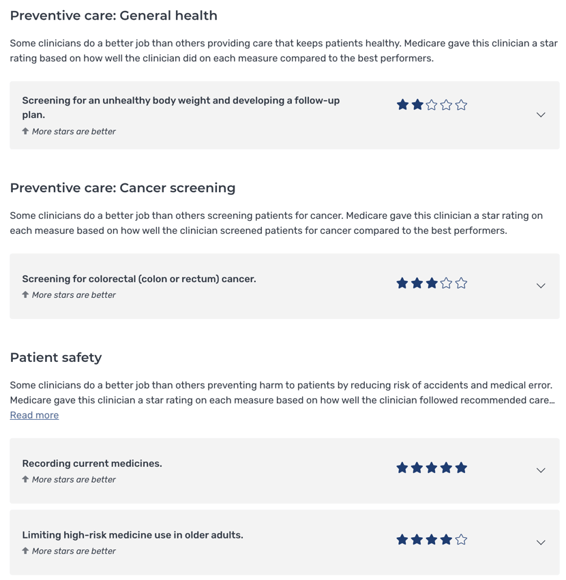
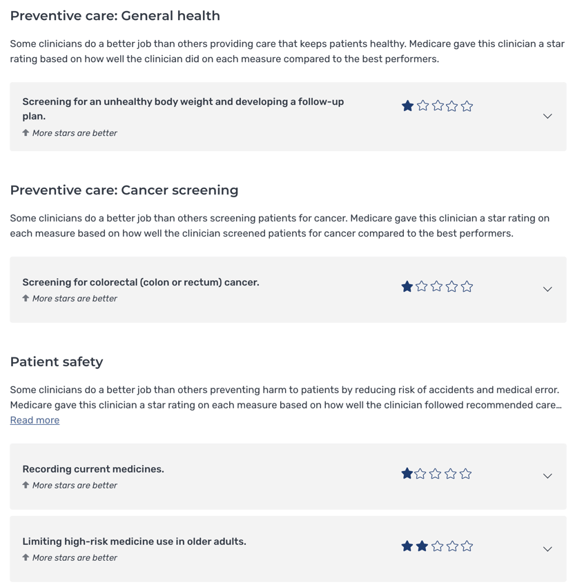
Reputation with patients. As a patient looking for a doctor, I can now go to www.medicare.gov/care-compare/ and see provider performance star ratings. This is essentially YELP for healthcare providers and it’s fueled by MIPS scores. Initially there were very few measures being reported on this site, however CMS is adding additional measures to this site every year.
As an example, if a patient is looking for a physician, looking up two different physicians in my area, I see the following for two physicians. All other things being equal, I’d call the second physician for an appointment. An article in Health Affairs cited that patients will pay an average of $3,152 for an additional star on a provider rating.
Value based contracts with commercial payers – MIPS, and your use of MIPSpro, are a strategic on-ramp to value-based care contracts with commercial payers. Every large commercial payer is encouraging providers to move to value-based care contracts with shared savings opportunities. Data analysis is an essential part of a value-based payment arrangement, offering providers a deeper understanding of their patients and their care needs, including all the interactions they’ve had with the healthcare system. Additionally, data are used to determine needed improvement on performance metrics.
MIPS has required providers to analyze and report data across all payers for the last four years. MIPSpro users collect quality data and have access to cost data that informs negotiating and succeeding at contracts with commercial payers. We have the data and can assist in analysis, negotiating, and achieving ROI in these contracts.
Alternative Payment Models within CMS – CMS has made it clear that APMs are the future of payment for services, and the goal is to move providers out of FFS / MIPS into these programs by 2030. While 2030 can seem like a long way off, there are steps to take to evaluate the programs, determine the best fit, and transition. The data in MIPSpro assists in evaluating the path forward.
The ROI on your MIPSpro efforts go beyond the penalty avoidance and incentive you see in the MIPS program for your efforts. Contact us to schedule a time to discuss your strategic goals and let us assist in achieving them.

