2024 stands as a pivotal year for healthcare providers, marking the end of leniency granted since the COVID-19 Public Health Emergency began. Participation in the Quality Payment Program (QPP) and the Merit-based Incentive Payment System (MIPS) is no longer optional — if providers fail to engage, they’ll face penalties.
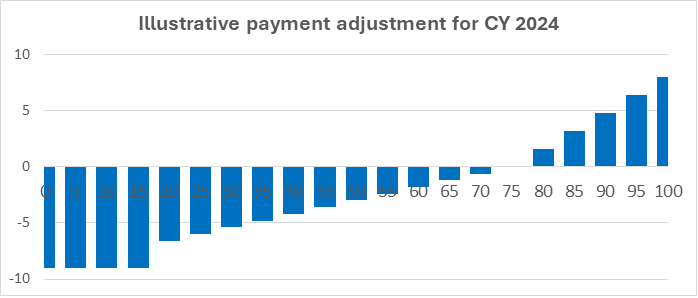
Over the past 4 years, exemptions were readily available, allowing providers to sidestep penalties. Those who participated in the program were enticed with incentives reaching up to 8.25%. Meanwhile, providers at risk of low scores or those disinclined to participate could opt out without repercussion. CMS also noted that many providers who participated submitted exemptions in categories where their performance was low, leading to inflated final total scores.
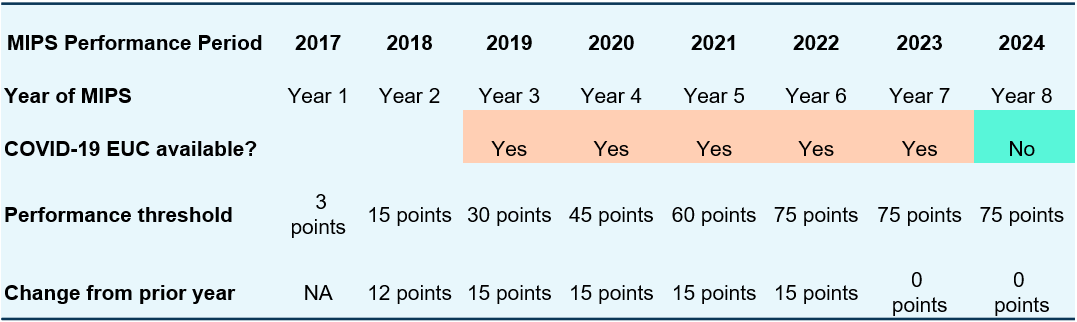
In 2024, MIPS will be fully enforced for the first time since 2019. After years of inactivity, numerous clinicians will find themselves ill-equipped to engage in 2024. CMS projects that 22% of clinicians will face penalties this year.
Regardless of the reporting solution employed, substantial effort will be required to evade penalties and achieve incentives in 2024. Consequently, 2024 should result in a significant MIPS bonus pool, rewarding those who are prepared and committed to delivering quality work.
As participants re-enter the program, they’ll find a drastically changed landscape. The QPP/MIPS program has evolved, growing more complex and retiring many policies that helped program participants boost their scores in prior years. Notably, bonus points have been eliminated, performance benchmarks for measures have escalated, and a mandatory Cost performance category has been added to scoring.
Data submission requirements have also increased. The data completeness threshold for the Quality performance category is now 75%. Promoting Interoperability data requirements have also grown.
In addition, the Centers for Medicare & Medicaid Services (CMS) have introduced an alternative route known as MIPS Value Pathways (MVPs). This program offers diverse options for engagement and potential greater success within the program. CMS estimates that 14% of clinicians who currently participate in MIPS will submit data for the measures and activities in an MVP during 2024. Deciphering the optimal route and whether to participate in this pathway, however, isn’t straightforward.
For providers who’ve previously secured exemptions, the time to re-engage with the QPP/MIPS program is now. The 2024 performance year demands early and strategic planning to avoid penalties or maximize potential incentives. Act promptly to determine your participation strategy, ensure compliance with the new program requirements, and maximize reimbursement from CMS.
There are 3 ways to check your QPP/MIPS eligibility for 2024
1. Use the QPP participation status tool on the QPP website at to check eligibility for a single clinician.

2. Sign in to the QPP website to check eligibility for multiple clinicians.

Who is considered a MIPS-eligible clinician?
1. Eligible clinician types: Physicians (including doctors of medicine, osteopathy, dental surgery, dental medicine, podiatric medicine, and optometry), osteopathic practitioners, chiropractors, physician assistants, nurse practitioners, clinical nurse specialists, certified registered nurse anesthetists, physical therapists, occupational therapists, clinical psychologists, qualified speech-language pathologists, qualified audiologists, registered dietitians or nutrition professionals, clinical social workers, and certified nurse midwives are eligible clinician types.
2. The Low-Volume Threshold: You’re considered a MIPS-eligible clinician (i.e., required to report) and will receive a payment adjustment when you’re enrolled in Medicare before Jan. 1, 2023. You exceed the Low-Volume Threshold if you bill more than $90,000 and provide care for more than 200 Medicare Part B patients or have more than 200 covered professional services.
Possible exemptions
- Newly enrolled in Medicare: If a clinician enrolls in Medicare in the middle of a performance year, they don’t have to participate in MIPS reporting that year.
- The Low-Volume Threshold: Otherwise eligible clinicians or groups are exempt from MIPS reporting if they bill $90,000 or less, provide care for 200 or fewer Medicare Part B patients, or have 200 or fewer covered professional services. They may opt in or voluntarily report if they want to participate in the incentive program or monitor their performance for other reasons.
- Advanced APM participation: For the 2023 performance year, if you have a certain percentage of your Part B payments through an Advanced APM or see a certain percentage of your patients through an Advanced APM, you won’t have to submit data to MIPS.
There is no exemption for COVID-19 impact for 2024. The exemption to request reweighting of MIPS performance categories due to COVID-19 has been retired.
About Healthmonix
Healthmonix is at the leading edge of MIPS participation, optimization, and reporting. We’ve enabled providers to fine-tune their performance and reporting strategies, securing over $200 million in annual incentives and avoiding over $500 million in penalties in just one year. Our advanced reporting engines are designed to help providers select and implement the most advantageous reporting options.
Check out our webinar on the 2024 quality measures. Register here.

