On October 14, 2016, the Department of Health and Human Services release the MACRA Quality Payment Program Final Rule. According to the Executive Summary of the Final Rule, the aims of the Quality Payment Program are to : "(1) support care improvement by focusing on better outcomes for patients, decreased provider burden, and preservation of independent clinical practice; (2) promote adoption of Alternative Payment Models that align incentives across healthcare stakeholders; and (3) advance existing efforts of Delivery System Reform, including ensuring a smooth transition to a new system that promotes high-quality, efficient care through unification of CMS legacy programs."[1]
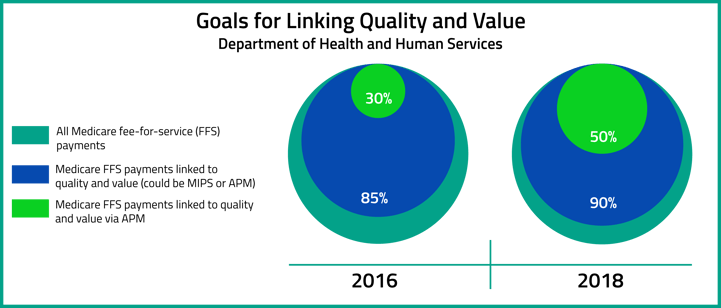
Consistent with what was discussed in the proposed rule making, the MACRA Quality Payment Program will be split into two tracks; the Merit-Based Incentive Payment System (MIPS) and Advanced Alternative Payment Models (Advanced APMs). CMS predicts that for the first year that the MACRA Quality Payment program is implemented, most eligible clinicians will participate in MIPS. However, participation in Advanced APMs is both expected and encouraged to grow in the years to come. CMS currently estimates that by performance year 2018, Advanced APM participation will account for 50% of all clinicians participating in the Quality Payment Program. We have previously discussed MIPS at great length, and today our purpose is to answer the biggest questions concerning Advanced APM participation.
 What are Alternative Payment Models (APMs)?
What are Alternative Payment Models (APMs)?
As defined on the new and improved CMS Quality Payment Program website, an Alternative Payment Model, or APM, is a payment approach that incentivizes providing high-quality and cost-efficient care. They are a part of how CMS envisions their efforts of shifting from volume-based care to value-based care being actualized. APMs generally apply to a specific clinical condition, a care episode, or a patient population.
In certain situations, APMs can qualify as Advanced APMs. Clinicians that are a part of a qualified Advanced APM are considered Qualifying APM Participants (QPs) and are exempt from participating in MIPS.
 What APM models will qualify as Advanced APMs?
What APM models will qualify as Advanced APMs?
There are two types of Advanced APMs, called by CMS Advanced APMs and Other Payer Advanced APMs. Other Payer Advanced APMs allow for arrangements to be made with other payers, such as Medicaid or a commercial payer. For an APM to qualify as an Advanced APM, it must meet the following three criteria:
- The use of CEHRT must be required by the APM
- Payments and quality measures must be tied together in a way that is comparable to the quality performance category under MIPS
- The APM must either be a Medical Home Model or assume more than a nominal amount of monetary risk for the APM entities
 How do I participate in an Advanced APM?
How do I participate in an Advanced APM?
To participate in an Advanced APM, you must locate a qualified Advanced APM, and inquire about how to apply. The initial determination for APMs that will qualify as Advanced APMs for the 2017 performance year has been made. This list is subject to change, and will be finalized by January 1, 2017.
- Comprehensive ESRD Care (CEC) - Two-Sided Risk
- Comprehensive Primary Care Plus (CPC+)
- Next Generation ACO Model
- Shared Savings Program - Track 2
- Shared Savings Program - Track 3
- Oncology Care Model (OCM) - Two-Sided Risk
We will be writing more about what participation looks like for each model of Advanced APMs, so to learn more, you can subscribe to updates!
Citations
[1] The Department of Health and Human Services. (2016, Oct. 14). Executive Summary; Medicare Program; Merit-based Incentive Payment System (MIPS) and Alternative Payment Model (APM) Incentive under the Physician Fee Schedule, and Criteria for Physician-Focused Payment Models. Retrieved from https://qpp.cms.gov/docs/QPP_Executive_Summary_of_Final_Rule.pdf
[2] Medicare Program; Merit-Based Incentive Payment System (MIPS) and Alternative Payment Model (APM) Final Rule, 42 CFR § 414 (2016). [CMS-5517-FC]
[3] Medicare Program; Merit-Based Incentive Payment System (MIPS) and Alternative Payment Model (APM) Proposed Rule, 42 CFR § 414 (2016).

