The proposed rule for the implementation of MACRA and its underlying Quality Payment Program has inspired many clinicians to voice their opinions about how excessive reporting leads to a reduction in the quality of patient care, and how the rule disadvantages small and rural practices. Two months ago, in response to this feedback, Andy Slavitt announced to senate that there was a possibility of a MACRA delay, or some restructuring of the proposed rule to reduce the burden of compliance. On Thursday, September 8, CMS announced that providers will be able to choose the level and pace at which they will comply with MACRA.
Approximately 90% of MACRA eligible clinicians are anticipated to participate in the Merit-Based Incentive Payment System (MIPS) because of the risk associated with not qualifying as an Advanced Alternative Payment Model (APM). On Thursday, CMS introduced three levels of MIPS compliance that should ease the burden for at least the first year of MACRA's Quality Payment Program.
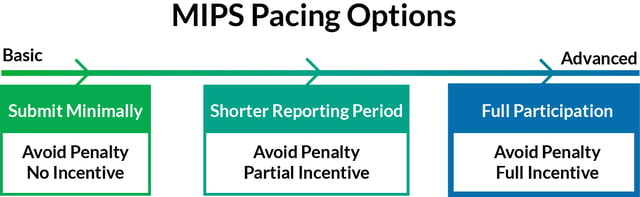
 Minimal participation in the MIPS Quality Payment Program
Minimal participation in the MIPS Quality Payment Program
Financial Impact: Potential avoid the 4% penalty, no chance for incentive
This option was designed to ease providers into the process of MACRA compliance, designed with clinicians who are adopting new technology solutions in mind. Essentially, so long as a group or individual submits some Quality Payment Program data to CMS from after January 1, 2017, they will be able to avoid the 4% penalty to their 2019 claims. A full description of baseline submission requirements will be available in the final rule, scheduled for release in November 2016. Providers choosing this option should be mindful that they will be expected to participate more broadly for the 2018 and 2019 performance years if they elect this option for 2017.
 Participate fully in MIPS for a shortened reporting period
Participate fully in MIPS for a shortened reporting period
Financial impact: Potential to avoid the 4% penalty and for a partial incentive (actual incentive percentage to be defined in November as a part of the final rule).
This option is best for clinicians that are comfortable with quality reporting (previously PQRS), but unsure about their preparedness to comply for a full calendar year. It allows clinicians to report data to CMS for a period of time shorter than a full calendar year, so long as that custom reporting period begins after January 1,2017. Further information, such as the minimum length of time that will be considered an eligible reporting period, will be available with the release of the final rule.
 Full MIPS Participation for the 2017 Calendar Year
Full MIPS Participation for the 2017 Calendar Year
Financial impact: Potential to avoid the 4% penalty and get a full incentive (up to 32%),
This option is for practices that are confident in their MIPS reporting strategy. Under this option, practices will comply with MIPS as it is written in the final rule, which should closely align with the proposed rule from April.
After the April Quality Payment Program Proposal was released, provider organizations, along with medical groups like the American Medical Association, the American Academy of Family Physicians and the Medical Group Management Association, campaigned the Department of Health and Human Services for more flexibility with MACRA implementation. These pacing options were announced to facilitate the needs expressed from this feedback. In addition to these three options for MIPS participation, the option of participating in a qualifying APM, such as the Medicare Shared Savings Program Accountable Care Organization (MSSP ACO), is still an option for Quality Payment Program participation.
Sources:
[1] via CMS, Plans for the Quality Payment Program in 2017: Pick Your Pace
[2] via Modern Healthcare, CMS will give providers flexibility on MACRA requirements

 Participate fully in MIPS for a shortened reporting period
Participate fully in MIPS for a shortened reporting period