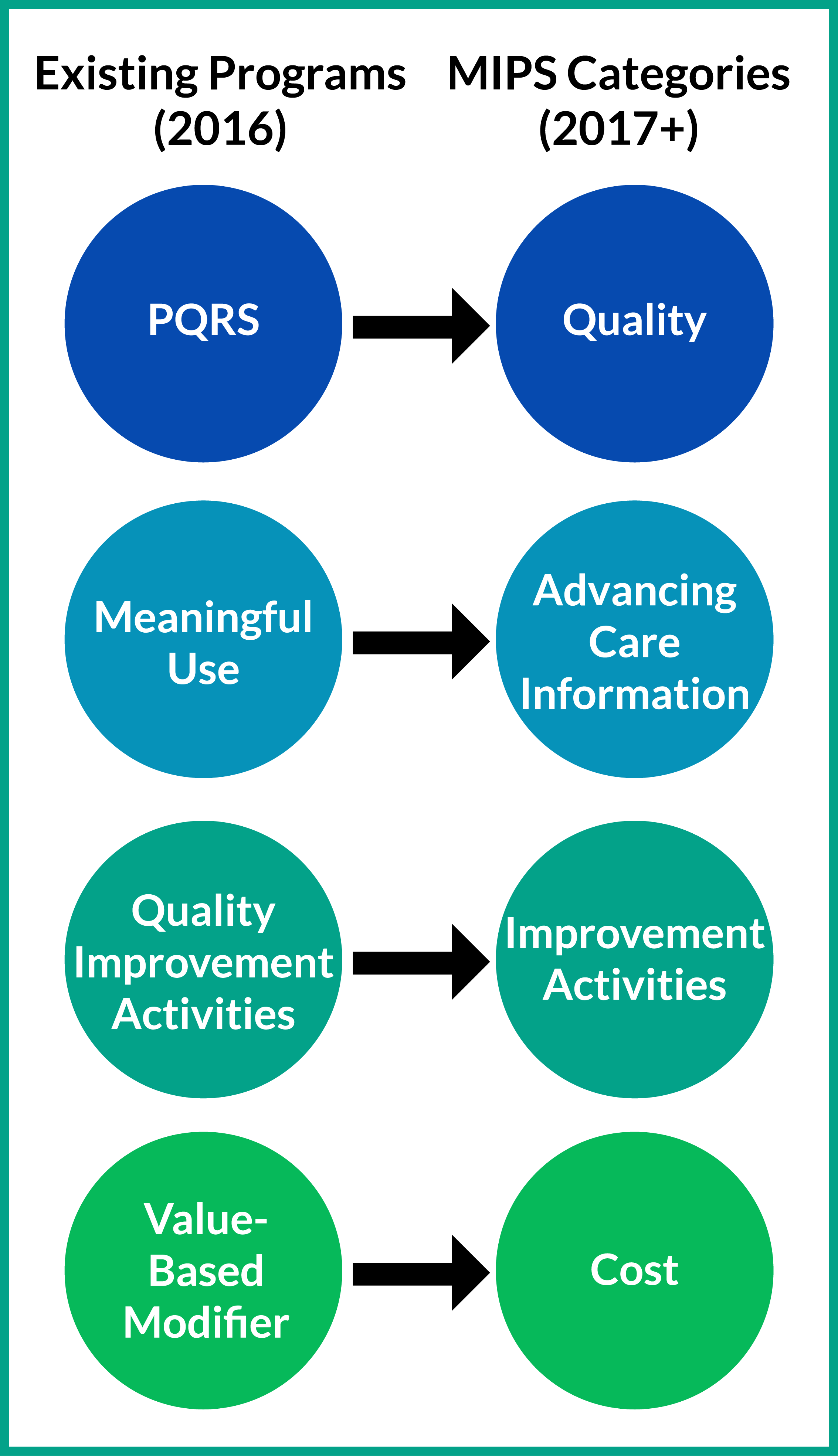
With the beginning of June came the half-way point for the first year of MIPS reporting. While many providers haven't started reporting yet, a good number of clinicians have started early. We interviewed clinicians and practice administrators who have reported PQRS in the past via registry, are currently reporting through the MIPSPRO registry, and that represent a diverse demographic of MIPS eligible clinicians.
Topics: PQRS, MACRA & MIPS, Industry insights, Small Practice, Hospitals & Health Systems
The Improvement Activities Performance Category of MIPS is the the newest quality improvement initiative from CMS. Reporting this category is relatively simple, entailing only that eligible clinicians or groups attest to completing between one and four out of 92 pre-selected improvement activities. Selecting Improvement Activities and understanding how the impact your MIPS final score can be tricky. Luckily, it doesn't have to be!
Topics: PRO Tips, MACRA & MIPS, Policy, IA Performance Category
During the first year of MIPS, it is deceptively easy to avoid the penalty. In a CMS blog post released a few weeks before the final rule was published, the Acting Administrator for CMS, Andy Slavitt, announced that there would be MIPS pacing options to allow eligible clinicians to ease into the program. The most basic level of reporting, referred to sometimes as the MIPS Test Option, is so simple to complete that it absolutely seems to good to be true.
Topics: PRO Tips, MACRA & MIPS, Physician Compare
One of the trickiest aspects of the new CMS Quality Payment Program is understanding how to report MIPS as a group. MIPS group reporting is when a TIN of 2 or more providers decides to report their MIPS measures and activities on the group (TIN) level, rather than on the individual (TIN+NPI) level. This could be an advantage to a practice that has a few providers who struggle to find measures that are relevant to them personally, or a practice exercising the "test option" of MIPS reporting for 2017. Eligible Clinicians must report either individually or as a group consistently across all MIPS performance categories.
Topics: MACRA & MIPS, Policy, Eligibility
The first performance year of the Merit-based Incentive Payment System (MIPS) is well underway. One of the most marked differences between MIPS and previous CMS initiatives is the quality of educational resources available to eligible clinicians. However, wading through all the different documents can be confusing if you are just starting out. This article will walk you through the available resources for each step of your MIPS educational journey.
Topics: MACRA & MIPS, CMS
House Republicans narrowly passed their long-promised Affordable Care Act repeal and replacement bill this Thursday. The American Healthcare Act barely scraped by with a vote of 217-213, with all 2017 "yes" votes coming from Republican Representatives. Although 20 Republican Representatives still opposed the bill, the revisions were able to convert 23 hard line conservatives into voting favorably. This proved enough for passage.
Topics: Policy
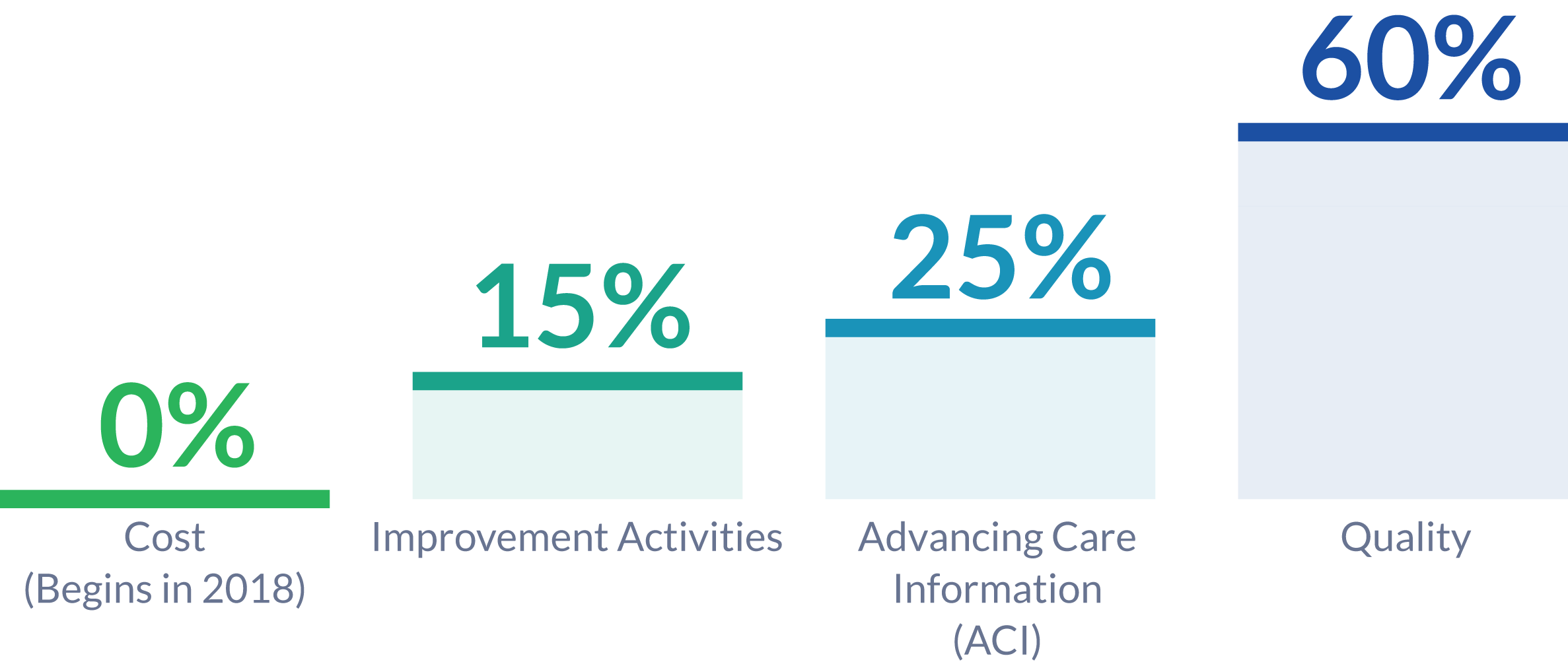
The Improvement Activities Performance Category is a new concept introduced by MIPS reporting and rewards eligible clinicians for participating in activities related to their patient population. Clinicians and groups can choose to participate in activities most relevant to both their practice and patient population. The Improvement Activities Performance Category is worth 15% of the MIPS Composite Performance Score in 2017.
Topics: MACRA & MIPS, Policy, IA Performance Category
The Advancing Care Information (ACI) Performance Category is Meaningful Use updated to be more flexible, customizable, flexible and focused on patient engagement and interoperability. ACI is worth 25% of your MIPS Composite Performance Score.
Topics: MACRA & MIPS, Policy, ACI Performance Category
The Quality Performance Category
The Quality Performance Category is one of four Performance Categories to be reported for the Merit-Based Incentive Payment System (MIPS). Carrying the highest weight of the four Performance Categories, the Quality Score will determine 60% of the MIPS Composite Performance Score for eligible clinicians or groups.
Topics: MACRA & MIPS, Policy, Quality Performance Category
Although the president has stated that he is moving on to other issues, the GOP remains hopeful that they will dismantle and replace the Affordable Care Act (ACA) in the not-too-distant future. The Republican's proposed replacement bill, the American Health Care Act (AHCA) was withdrawn last Friday as it lacked the votes to pass. Under pressure from conservative activists this week, House Republicans and the White House have renewed their efforts to repeal the Affordable Care Act and replace it with their own bill.
Topics: Policy