On Tuesday April 24th, CMS released a proposed rule which essentially overhauls the Medicare and Medicaid Electronic Health Record Incentive Programs (also known as the “Meaningful Use” program). The proposed rule includes updates to Medicare payment policies and rates under the Inpatient Prospective Payment System (IPPS) and the Long-Term Care Hospital (LTCH) Prospective Payment System (PPS). Here are five things you should know about the proposed changes:
CMS Proposes Overhauling Meaningful Use: 4 Important Takeaways
Topics: CMS, Interoperability, Policy, ACI Performance Category, PI Performance Category
Last week’s 2018 HIMSS Conference presented, as every year, a profusion of insights into the current landscape of healthcare technology. With over 300 education sessions, 1,300 vendors, and hundreds of special programs and events, a HIMSS conference can be hard to boil down into just a few key points. Still, I wanted to share one particularly salient impression that stuck with me after I attended, one that I think anyone with an interest in healthcare should stick a pin in.
Topics: CMS, Industry insights
Interested in providing feedback to CMS about the burden that MIPS places on your practice?
Apply to help CMS in its new study, running from April 2018 through March 2019, and make your voice heard.
CMS is looking for groups and individuals that are eligilbe for MIPS to help study the burden that the MIPS program, particularly the Quality component, place on eligible clinicians. In return, successful participants will receive full credit for the Improvement Activity component of MIPS this year (2018).
Topics: MACRA & MIPS, CMS, Quality Performance Category, Administrative Burden
In late October, CMS launched a new initiative, Patients Over Paperwork, targeted to reduce unproductive regulatory burdens on health care providers and increase efficiency. CMS Administrator Seema Verma announced the initiative during a stakeholder meeting with more than 30 industry groups.
The initiative is potentially wide reaching, affecting a broad range of regulations surrounding practices such as prior authorizations, documentation of evaluation and management codes, OIG audits, and EHR requirements.
According to Verma, this has already touched the QPP final rule for 2018. As an outcome of this initiative, the QPP final rule includes policies that exclude individual MIPS eligible clinicians with less than or equal to $90,000 in Part B allowed charges or less than or equal to 200 Part B beneficiaries.
Topics: CMS
On October 30, CMS Administrator Seema Verma announced the Meaningful Measures initiative, which is intended to streamline quality reporting. This initiative is meant to address common criticisms of today’s performance measures, including their excessive focus on evaluating processes and the lack of alignment between programs. According to Verma, “Meaningful Measures will involve only assessing those core issues that are the most vital to providing high-quality care and improving patient outcomes.”
Topics: CMS
We are now in the seventh month of the new Merit-Based Incentive Payment System (MIPS), and the majority of MIPS-eligible clinicians still feel completely unprepared for success. With complicated and changing regulations, ensuring compliance can be a long and arduous process. Like most sizable goals, MIPS is best digested in small pieces, but it is hard to tell where to start sometimes. That is why we are going give you an order of operations to follow to ensure MIPS survival.
Topics: PRO Tips, MACRA & MIPS, CMS, Eligibility
Transparency is a vital aspect of the transition to quality care because it allows patients to make more informed healthcare choices. To this end, CMS has increased accessibility of physician information with the Physician Compare website, which publicly reports provider data including some quality measures. If you are a provider and want to assess or even optimize how you appear compared to your peers, you may have questions about how the Physician Compare website works and how to make sure it represents you accurately.
Topics: MACRA & MIPS, CMS, Physician Compare, Policy
The first performance year of the Merit-based Incentive Payment System (MIPS) is well underway. One of the most marked differences between MIPS and previous CMS initiatives is the quality of educational resources available to eligible clinicians. However, wading through all the different documents can be confusing if you are just starting out. This article will walk you through the available resources for each step of your MIPS educational journey.
Topics: MACRA & MIPS, CMS
MIPSPRO by Healthmonix Awarded 2017 Qualified MIPS Registry Status by CMS
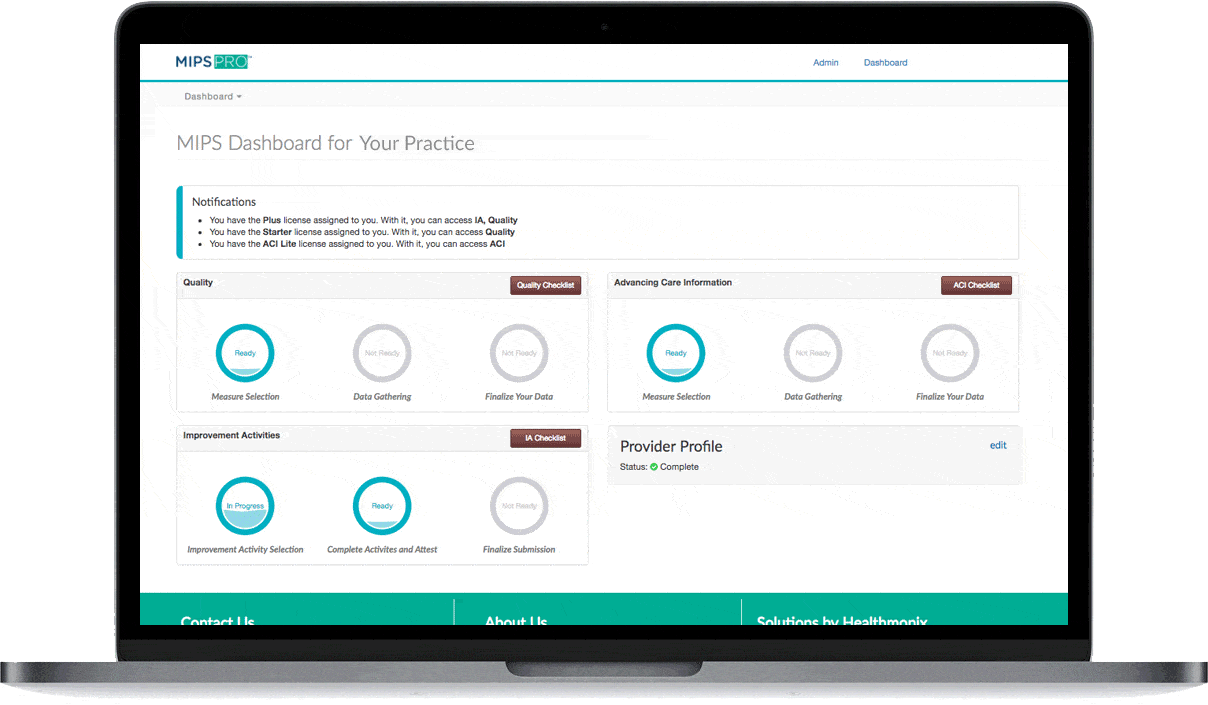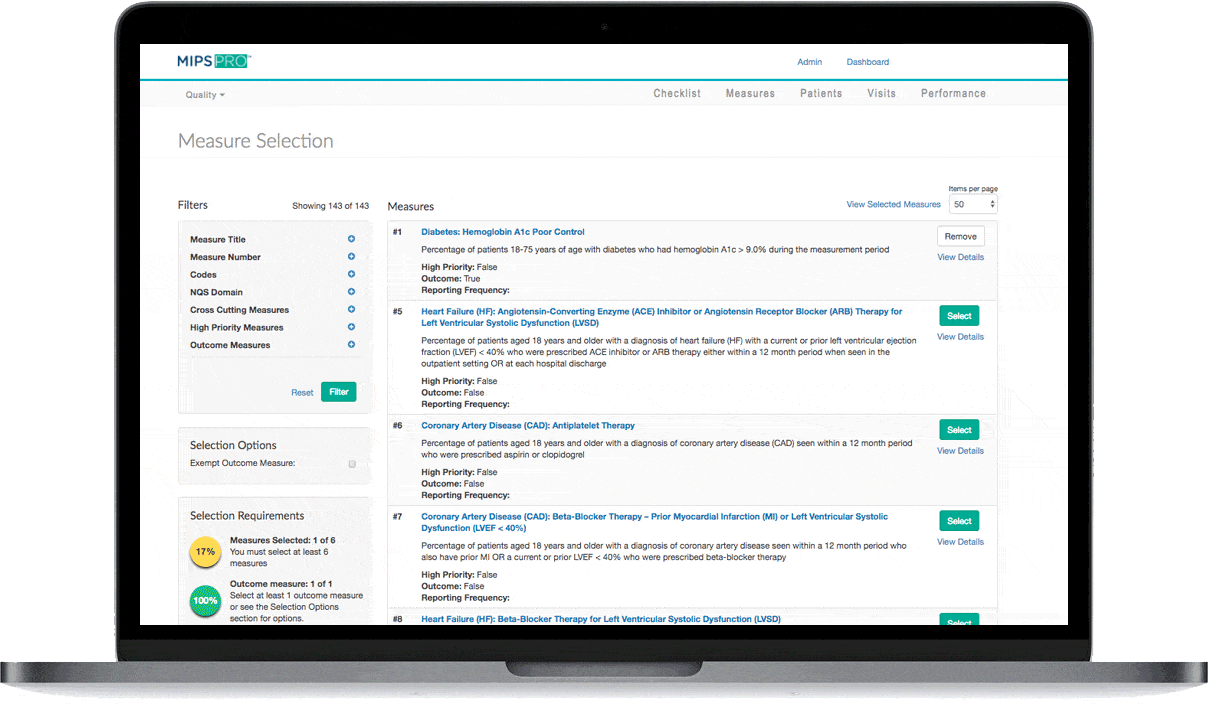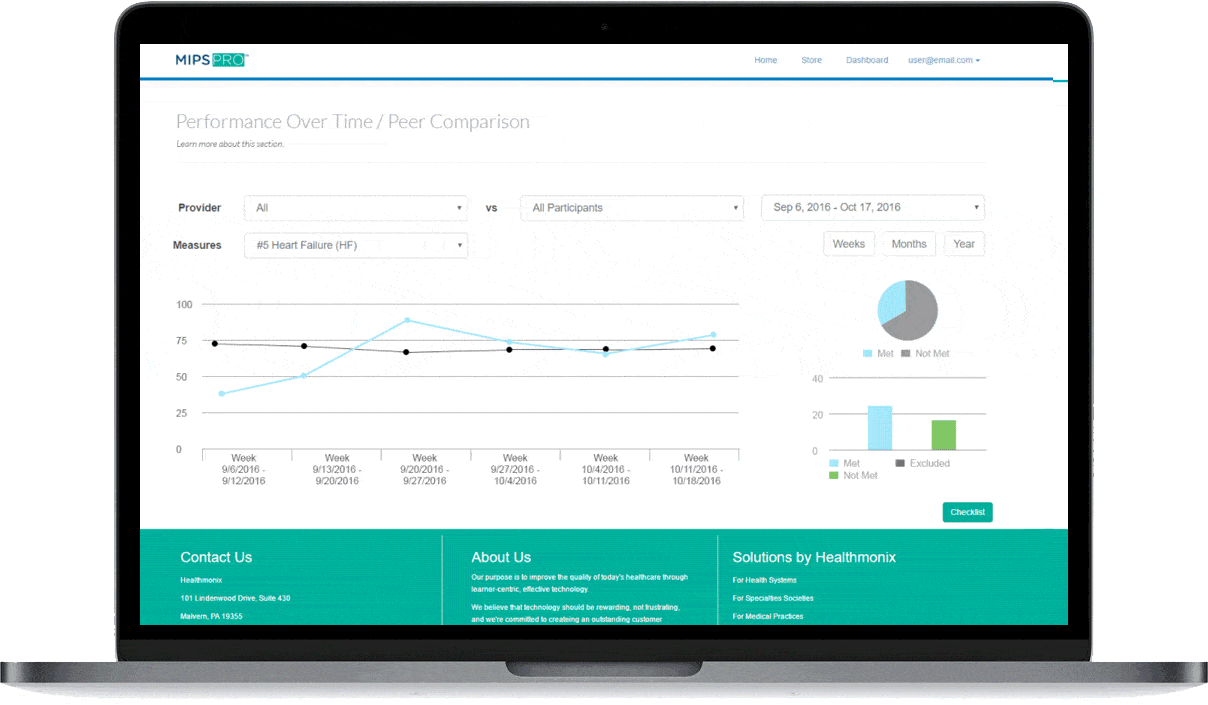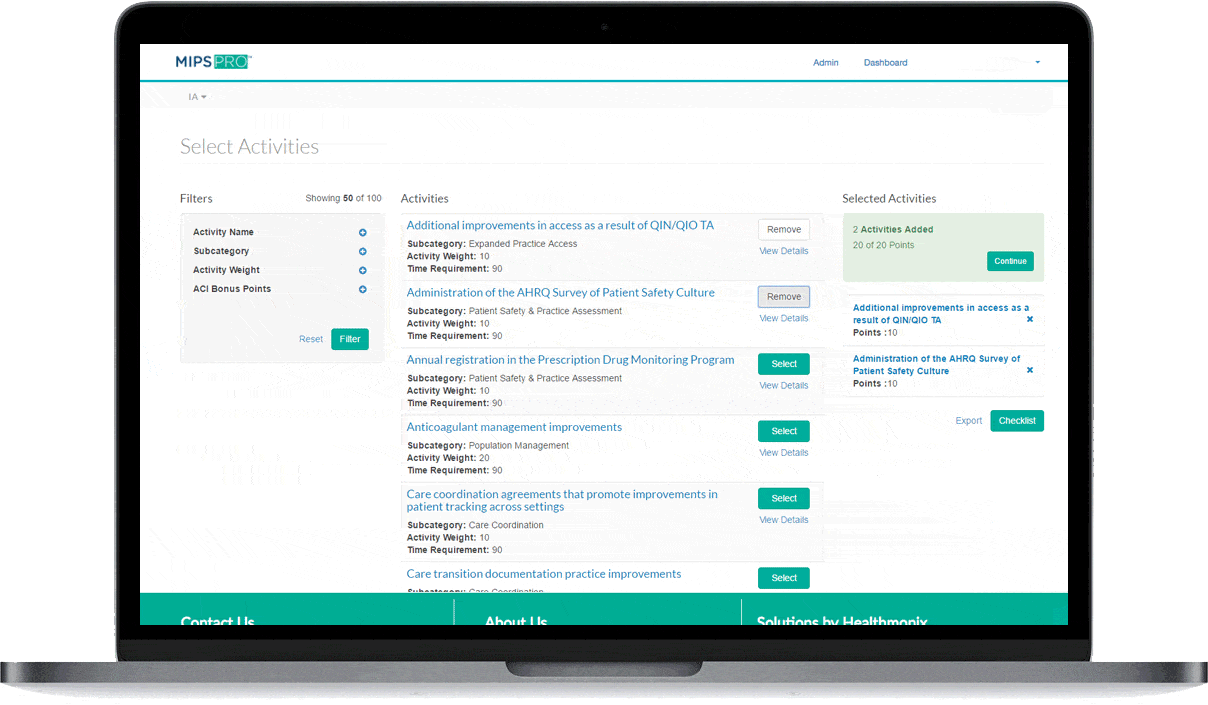
Malvern, PA – March 16, 2017 – Healthmonix was first-to-market with an all-inclusive solution for MIPS reporting, MIPSPROTM. This Qualified MIPS Registry is an end-to-end reporting solution, supporting the Quality, Advancing Care Information, and Improvement Activity Performance Categories of the Merit-Based Incentive Payment System (MIPS). The MIPSPRO engine also provides sophisticated real-time performance analytics, critical to competing for top MIPS incentives and improving patient outcomes.
Topics: MACRA & MIPS, CMS, Healthmonix
Compared to the commotion surrounding other Trump administration nominees, Seema Verma's confirmation hearing passed by last Thursday with relatively little controversy. Despite the low level of coverage, understanding the contents of this hearing is imperative for predicting the next few years in American health care. As the Administrator for the Centers for Medicare and Medicaid Services (CMS), Seema Verma will shape the future of health care for 34% of Americans. [1]
Topics: MACRA & MIPS, CMS